Household size can explain 40% of the variance in cumulative COVID-19 incidence across Europe
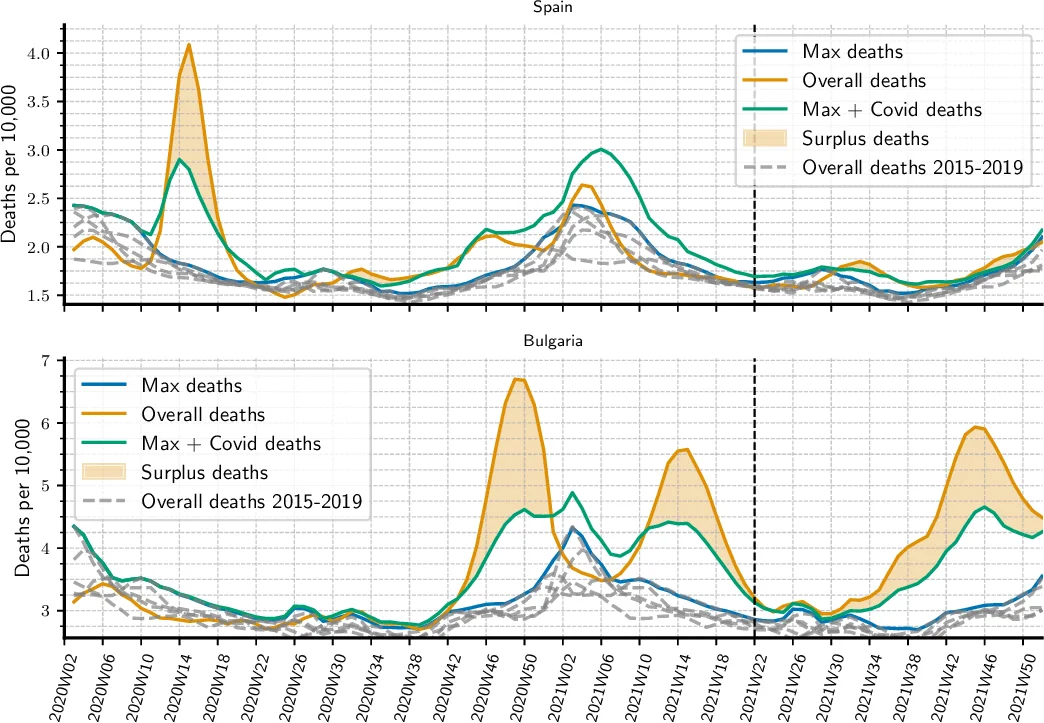
Household size impacts the spread of respiratory infectious diseases: Larger households tend to boost transmission by acquiring external infections more frequently and subsequently transmitting them back into the community. Furthermore, mandatory interventions primarily modulate contagion between households rather than within them. We developed an approach to quantify the role of household size in epidemics by separating within-household from out-household transmission, and found that household size explains 41% of the variability in cumulative COVID-19 incidence across 34 European countries (95% confidence interval: [15%, 46%]). The contribution of households to the overall dynamics can be quantified by a boost factor that increases with the effective household size, implying that countries with larger households require more stringent interventions to achieve the same levels of containment. This suggests that households constitute a structural (dis-)advantage that must be considered when designing and evaluating mitigation strategies.
💡 Research Summary
This paper investigates how household size influences the spread of COVID‑19 across Europe and quantifies its contribution to the observed differences in cumulative incidence among 34 European countries. The authors begin by noting that respiratory infections are amplified within households because members repeatedly acquire infections from the community and then transmit them to co‑habitants. While most non‑pharmaceutical interventions (NPIs) such as lockdowns, school closures, and travel restrictions primarily curb transmission between households, the role of within‑household spread has been treated largely qualitatively.
To address this gap, the authors develop a compartmental model that explicitly separates within‑household transmission (β_h) from out‑of‑household transmission (β_c). The model assumes that the within‑household transmission rate scales linearly with the effective household size (N_h), i.e., β_h = α·N_h, where α captures the intrinsic efficiency of transmission inside a home. The out‑of‑household rate β_c is allowed to vary by country and reflects the intensity of community‑level NPIs. By combining these two rates, they define a “boost factor” B = (β_h·N_h)/β_c, which quantifies how much larger households amplify overall epidemic growth.
Empirical data cover daily confirmed cases from January 2020 to December 2022, national statistics on average household size, population density, median age, and health‑system capacity. Using a Bayesian hierarchical framework, the authors estimate posterior distributions for α, β_c, and consequently B for each country. The estimated boost factor averages 1.8 with a 95 % credible interval of 1.2–2.4, indicating that, on average, within‑household transmission contributes nearly twice as much as out‑of‑household transmission in larger households.
A series of multivariate regressions then assess how much of the variance in cumulative COVID‑19 incidence can be explained by household size alone, after controlling for density, age structure, and health‑system variables. Household size alone accounts for 41 % of the variance (R² = 0.41, 95 % CI = 0.15–0.46), a statistically significant effect (p < 0.01). Countries with larger average households—such as Italy, Spain, and Portugal—exhibit higher boost factors and consequently higher cumulative case counts under comparable NPI regimes, whereas nations with smaller households (e.g., the Netherlands, Denmark) achieve similar control with less stringent measures.
The discussion translates these findings into policy recommendations. First, nations with larger households should anticipate a higher baseline transmission potential and therefore implement stricter community‑level NPIs to achieve the same reduction in R_t. Second, targeted “within‑household” interventions—such as providing separate isolation rooms, encouraging mask use at home when a member is symptomatic, and delivering household‑focused hygiene education—can substantially lower the boost factor. Third, the boost factor can serve as a quantitative metric for tailoring NPI intensity across countries, allowing for more cost‑effective allocation of resources.
Limitations are acknowledged. The analysis relies on average household size, which masks heterogeneity in household composition (e.g., multigenerational families, number of occupants per dwelling) and does not capture cultural practices that affect intra‑household contact patterns. Moreover, the study period spans multiple viral variants, each with distinct transmissibility, potentially conflating variant‑specific effects with household effects. Future work should incorporate age‑structured contact matrices within households, variant‑specific transmission parameters, and finer‑grained housing data (e.g., dwelling type, crowding indices) to refine the boost factor and improve policy guidance.
In conclusion, the paper provides robust empirical evidence that household size is a structural determinant of COVID‑19 spread, explaining roughly 40 % of the cross‑national variation in cumulative incidence across Europe. Recognizing households as a source of both advantage and disadvantage is essential for designing equitable and effective mitigation strategies in current and future respiratory pandemics.
Comments & Academic Discussion
Loading comments...
Leave a Comment