Transverse contributions to the longitudinal stiffness of the human foot
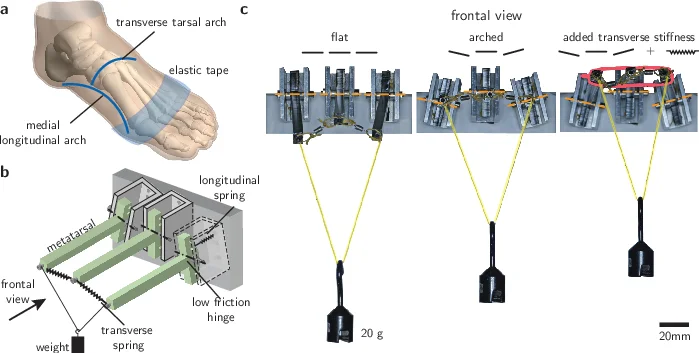
Humans rely on foot stiffness to withstand the propulsive forces of walking and running. Skeletal adaptations that increase foot stiffness include the medial longitudinal arch (MLA) and the transverse tarsal arch (TTA). The TTA has been hypothesized to stiffen the foot through cross-axis coupling of transverse intermetatarsal stiffness with sagittal-plane midfoot stiffness, but this has been tested only in cadaveric specimens. In vivo testing is essential because muscle contraction substantially modulates MLA function and may similarly affect the TTA’s cross-axis coupling. Here we provide in vivo evidence for the TTA’s contribution to foot stiffness by externally increasing intermetatarsal stiffness and measuring its effects on midfoot elasticity during walking. As predicted by the cross-axis coupling hypothesis, increasing intermetatarsal stiffness with an elastic tape wrapped around the forefoot reduced the energy absorbed in midfoot flattening and increased sagittal-plane midfoot stiffness concomitantly (mean,$\pm$,standard error of the mean (SEM): $13.9% \pm 3%$ and $16.8% \pm 5.8%$, respectively). However, taping did not change the curvature of the TTA, thereby isolating the effects of cross-axis coupling from morphological changes to the TTA. Thus, forefoot taping modulates midfoot stiffness through cross-axis coupling and could provide a non-invasive means to manage pathological foot flexibility or enhance athletic performance.
💡 Research Summary
The present study investigates whether increasing transverse intermetatarsal stiffness can augment longitudinal (sagittal‑plane) foot stiffness in vivo, thereby testing the cross‑axis coupling hypothesis that has so far been demonstrated only in cadaveric specimens. Thirteen healthy adults (5 females, 8 males, mean age ≈ 30 years) walked on a force‑measuring treadmill at a constant non‑dimensional speed while three experimental conditions were applied in random order: (1) a free condition with no tape, (2) a “taped” condition in which an elastic kinesiology tape was stretched to its maximum and wrapped tightly around the distal metatarsal heads, and (3) a “control” condition in which the same tape was applied loosely with negligible tension. The tape length was set to twice the unloaded forefoot circumference, and prior material testing on a dummy forefoot model quantified the added stiffness of the tape as 37.6 N mm⁻¹ ± 1.02 N mm⁻¹.
Three‑dimensional motion capture (500 Hz) and six‑axis ground‑reaction force data (2000 Hz) were recorded simultaneously. A multi‑segment foot model defined hind‑foot and fore‑foot segments, with the mid‑foot joint located at the midpoint between the navicular marker and the base of the fifth metatarsal. Inverse dynamics computed joint torques, forces, and power. Sagittal‑plane stiffness was quantified as the slope of the mid‑foot torque‑angle curve during dorsiflexion, while negative work (the time‑integral of negative power) measured the energy absorbed during mid‑foot flattening. Transverse arch curvature was assessed by the included angle between lines joining the first‑second and second‑fifth metatarsal bases projected onto the coronal plane; this metric remained unchanged across conditions.
The key findings were: (i) the taped condition reduced the negative work associated with mid‑foot flattening by 13.9 % ± 3 % relative to the free condition, indicating that less energy was dissipated when the foot was stiffer; (ii) sagittal‑plane stiffness, as reflected by the torque‑angle slope, increased by 16.8 % ± 5.8 % under the taped condition, confirming a stiffer response to the same dorsiflexion angle; (iii) transverse arch curvature did not differ between taped and free conditions, demonstrating that the observed stiffness changes were not due to geometric arch alterations but rather to the added transverse intermetatarsal resistance. Additionally, the inter‑metatarsal splay distance decreased from 9.4 mm ± 0.6 mm (free) to 5.6 mm ± 0.3 mm (taped), confirming that the tape effectively limited transverse spreading of the metatarsals.
Statistical analysis (repeated‑measures ANOVA with post‑hoc tests) showed all differences to be significant at p < 0.05, and repeatability was verified through dummy‑model testing and intra‑subject consistency checks. The authors interpret these results through a mechanical analogy: a curved transverse arch creates non‑parallel hinge axes; when the foot dorsiflexes, the metatarsals tend to splay, engaging transverse springs. By adding an external transverse spring (the tape), splay is restrained, which in turn raises the longitudinal stiffness—a classic cross‑axis coupling effect.
Clinically, the findings suggest that non‑invasive fore‑foot taping could be employed to mitigate excessive foot pronation or flat‑foot conditions by increasing transverse stiffness without altering foot shape. From a performance perspective, athletes might use targeted taping to enhance foot rigidity, thereby reducing energy loss during stance and potentially improving propulsion efficiency. The study acknowledges limitations, including the short‑term nature of the intervention, lack of direct muscle activation measurements, and the need for longitudinal studies to assess adaptation or fatigue effects.
In conclusion, this work provides the first in‑vivo experimental validation that augmenting transverse intermetatarsal stiffness via elastic taping leads to a measurable increase in sagittal‑plane foot stiffness, supporting the cross‑axis coupling hypothesis. The results enrich biomechanical models of foot function and open avenues for therapeutic and performance‑enhancing applications that exploit transverse‑to‑longitudinal stiffness interactions.
Comments & Academic Discussion
Loading comments...
Leave a Comment