Modeling the Effects of Multiple Myeloma on Kidney Function
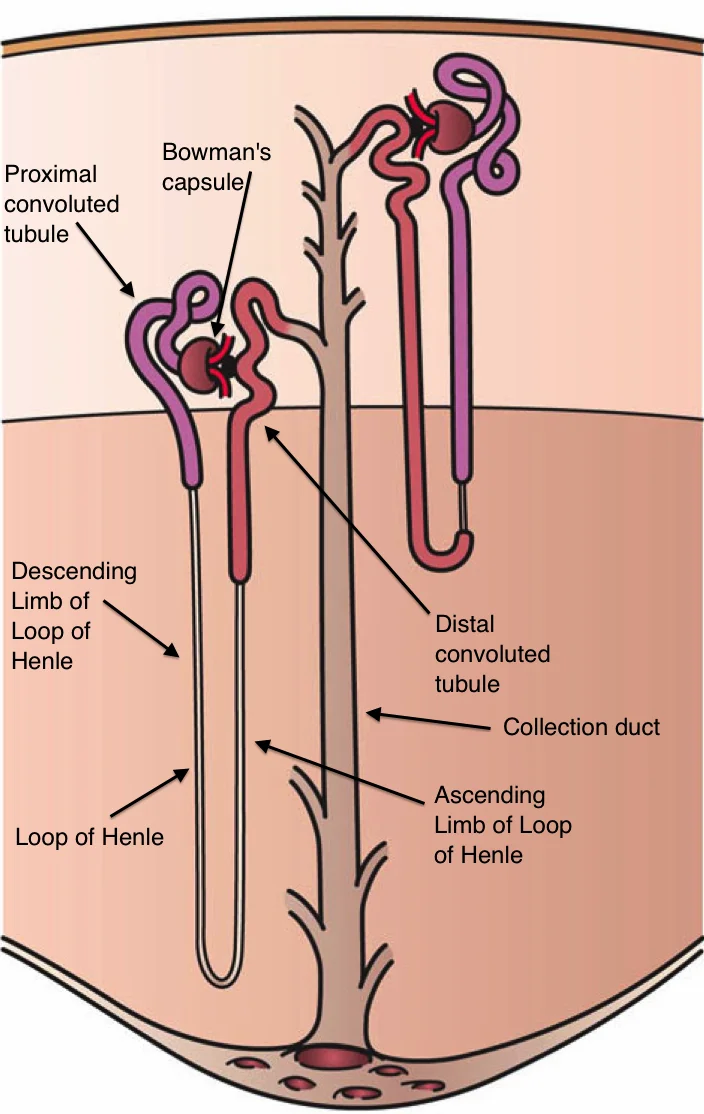
Multiple myeloma (MM), a plasma cell cancer, is associated with many health challenges, including damage to the kidney by tubulointerstitial fibrosis. We develop a mathematical model which captures the qualitative behavior of the cell and protein populations involved. Specifically, we model the interaction between cells in the proximal tubule of the kidney, free light chains, renal fibroblasts, and myeloma cells. We analyze the model for steady-state solutions to find a mathematically and biologically relevant stable steady-state solution. This foundational model provides a representation of dynamics between key populations in tubulointerstitial fibrosis that demonstrates how these populations interact to affect patient prognosis in patients with MM and renal impairment.
💡 Research Summary
The manuscript presents a novel deterministic mathematical framework that captures the key cellular and molecular interactions underlying tubulointerstitial fibrosis in multiple myeloma (MM) patients. The authors first construct a baseline model describing the dynamics of proximal tubule cells (PTCs), free light chains (FLCs), and renal fibroblasts in a healthy kidney. Using the Savageau‑Voit power‑law formalism, each population’s growth and death are expressed as nonlinear terms with biologically motivated exponents. In this normal‑kidney system, PTC proliferation is self‑limited and inhibited by rising FLC concentrations, FLCs are produced at a constant rate and cleared renally, and fibroblasts follow a logistic‑type growth limited by a maximal occupancy fraction.
To incorporate the malignant component, a fourth variable representing myeloma plasma cells (the tumor) is added. Tumor growth follows a Gompertz equation, reflecting a time‑dependent growth rate and a carrying capacity. The tumor contributes additional FLC production, and the model introduces EMT‑related terms that couple excess FLCs to PTC loss and fibroblast expansion, thereby creating a positive feedback loop that drives fibrosis. The resulting four‑equation system (PTC, FLC, fibroblast, tumor) is analyzed for steady‑states. Eight equilibria are identified, but only one satisfies biological plausibility (non‑zero PTC, FLC, fibroblast levels) and meets stability criteria (γ_F > µ_F, γ_L > µ_L, g₂ < 1).
Parameter values are drawn from published MM literature (particularly Ayati et al.) and supplemented with heuristic estimates to generate illustrative simulations. The authors demonstrate that, in the absence of tumor cells, the system settles to a stable healthy equilibrium. When the tumor term is activated, FLC concentrations rise sharply, PTC numbers decline, and fibroblast populations expand, reproducing the clinical trajectory toward tubulointerstitial fibrosis and eventual renal failure.
The paper’s strengths lie in its clear biological grounding, the use of power‑law kinetics that balance tractability with nonlinearity, and the systematic stability analysis that links mathematical conditions to physiological plausibility. It also provides a modular platform that can be extended to incorporate treatment effects (e.g., plasmapheresis, chemotherapy) or spatial heterogeneity across nephrons. However, several limitations are evident. Most parameters are estimated rather than calibrated to patient data, limiting quantitative predictive power. The model omits spatial structure, hemodynamic factors, and the stochastic nature of clonal evolution, which are important in MM progression. Sensitivity and uncertainty analyses are absent, leaving the robustness of the conclusions unclear. Moreover, the EMT representation is highly simplified, and the model does not differentiate between kappa and lambda light chains, which have distinct nephrotoxic profiles.
In conclusion, this work constitutes the first comprehensive mathematical description of MM‑induced renal tubulointerstitial fibrosis. It establishes a foundation for future efforts to integrate clinical biomarkers, personalize parameter estimation, and simulate therapeutic interventions. Such extensions could ultimately enable clinicians to predict renal decline in MM patients, tailor treatment timing, and improve overall survival outcomes.
Comments & Academic Discussion
Loading comments...
Leave a Comment