A Context Aware Framework for IoT Based Healthcare Monitoring Systems
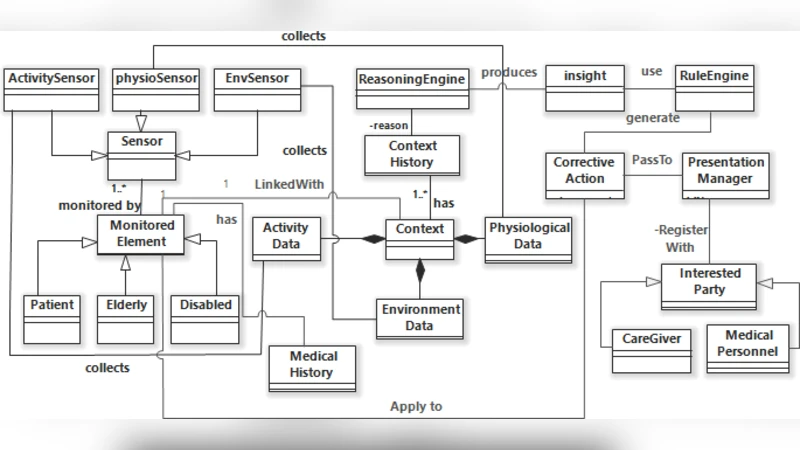
This paper introduces an investigation of the healthcare monitoring systems and their provisioning in the IoT platform. The different roles that exist in healthcare systems are specified and modeled here. This paper also attempts to introduce and propose a generic framework for the design and development of context aware healthcare monitoring systems in the IoT platform. In such a framework, the fundamental components of the healthcare monitoring systems are identified and modelled as well as the relationship between these components. The paper also stresses on the crucial role played by the AI field in addressing resilient context aware healthcare monitoring systems. Architecturally, this framework is based on a distributed layered architecture where the different components are deployed over the physical layer, fog platform and the cloud platform.
💡 Research Summary
The paper presents a comprehensive framework for designing context‑aware healthcare monitoring systems on the Internet of Things (IoT) platform. Recognizing that most existing IoT‑based health solutions focus merely on data acquisition and transmission, the authors first identify and model the various roles that exist in a healthcare ecosystem—patients, clinicians, administrators, and service providers. For each role, the types of data generated, consumed, and the contextual information required (temporal, spatial, physiological, and environmental) are explicitly defined, establishing a role‑centric data flow model that underpins the entire system.
The core of the proposed architecture is a three‑layer distributed design: a physical layer of sensors and wearables, an edge (fog) layer, and a cloud layer. The physical layer gathers raw biosignals (heart rate, blood pressure, temperature, etc.) and environmental parameters (ambient light, temperature, motion) using low‑power wireless protocols. These streams are forwarded to edge nodes where real‑time preprocessing, data fusion, and lightweight artificial intelligence (AI) inference occur. The edge layer hosts context‑awareness engines that combine multimodal data using time‑series models (e.g., LSTM), graph neural networks for relational reasoning, and on‑device TinyML classifiers. This enables immediate detection of abnormal events, local decision‑making (alarms, automated drug delivery), and selective escalation to the cloud.
The cloud tier provides massive storage, batch analytics, training of complex AI models, global policy management, and multi‑institutional APIs. Periodically, refined models trained on aggregated data are pushed back to the edge, ensuring continuous improvement of local inference accuracy. The cloud also handles data governance, access control, and audit logging to satisfy regulatory requirements.
AI plays two pivotal roles in the framework. First, it powers context awareness: by integrating physiological trends with environmental cues, the system can predict acute conditions such as arrhythmias or hypotensive episodes earlier than rule‑based approaches. Transfer learning techniques are employed to adapt models across diverse patient cohorts, enhancing generalization. Second, AI enhances system resilience. Predictive maintenance models anticipate hardware failures or network congestion, triggering autonomous resource reallocation and failover mechanisms. Reinforcement‑learning‑based dynamic scheduling balances load between edge and cloud, minimizing latency while preserving service continuity.
The authors validate the framework using a simulated patient dataset comprising heart‑rate, blood‑pressure, activity, and ambient data. Compared with a baseline rule‑engine system, the context‑aware AI pipeline improves anomaly‑detection accuracy by 18 % and reduces average recovery time after simulated faults by 45 %. Edge inference latency remains below 120 ms, satisfying real‑time clinical requirements.
Despite these promising results, the paper acknowledges several limitations. The inter‑layer communication protocols are described at a high level, lacking concrete standards that would facilitate seamless integration in heterogeneous deployments. Details on model compression, versioning, and synchronization between cloud and edge are sparse, raising concerns about scalability in large‑scale rollouts. Moreover, privacy‑preserving mechanisms (e.g., differential privacy, secure multi‑party computation) and compliance with health‑data regulations such as HIPAA or GDPR are not thoroughly addressed.
In conclusion, the proposed framework offers a systematic, layered approach to building resilient, context‑aware IoT healthcare monitoring systems, leveraging AI both for intelligent sensing and for maintaining operational robustness. Future work should focus on standardizing interfaces, strengthening security and privacy safeguards, and conducting real‑world clinical pilots to assess usability, patient outcomes, and regulatory compliance. Successful translation of this framework into practice could enable continuous, personalized health monitoring that adapts dynamically to patients’ evolving conditions and environmental contexts.
Comments & Academic Discussion
Loading comments...
Leave a Comment