Tumour Induced Angiogenesis and Its Simulation
Due to over-metabolism, the tumour cells become hypoxic. To overcome this situation tumour cells secret several chemical substrates to attract nearby blood vessels towards it (angiogenesis). Transition from avascular to vascular tumour is possible with the initiation of angiogenesis. Angiogenesis also plays a crucial role to spread the cancer cells and its colonization at the distant locations of the body (metastasis). In this paper, we briefly review the processes and factors which directly affect tumour angiogenesis or may get affected by it. A model based on cellular automata is developed to demonstrate this complex process through MATLAB based simulation.
💡 Research Summary
The paper provides a concise review of tumour‑induced angiogenesis and introduces a simple cellular automata (CA) model to simulate the sprouting process. It begins by describing how rapidly proliferating tumour cells become hypoxic once they outgrow their existing vasculature. Hypoxia stabilises hypoxia‑inducible factors (HIF‑1α and HIF‑2α), which in turn up‑regulate a suite of tumour‑angiogenic factors (TAFs) such as vascular endothelial growth factor (VEGF‑A), platelet‑derived growth factor (PDGF‑B), fibroblast growth factors (FGF‑1/2), and angiopoietins (ANG‑1, ANG‑2). The authors detail the downstream signalling pathways, receptor interactions (VEGFR‑1/2, FGFR, Tie‑2), and the resulting cellular behaviours: endothelial cell (EC) proliferation, migration, basement‑membrane degradation (via MMP‑2/9), pericyte recruitment, and eventual formation of capillary loops.
A complementary discussion of anti‑angiogenic molecules (angiostatin, endostatin, thrombospondins) highlights the delicate balance between pro‑ and anti‑angiogenic signals in normal physiology versus the dysregulated environment of cancer. The review also touches on alternative angiogenic mechanisms such as vasculogenic mimicry and lymphangiogenesis, though these are not explored in depth.
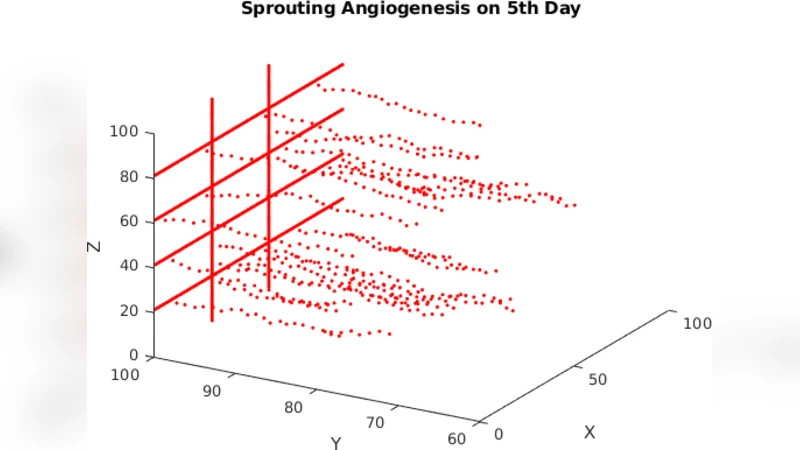
The core contribution is a CA‑based computational model implemented in MATLAB. The model represents a two‑dimensional lattice where each cell holds two state variables: (i) concentration of TAFs, governed by a diffusion‑decay equation, and (ii) presence or absence of a vessel segment. Tumour tissue is modelled as a fixed circular region that continuously secretes TAFs. When the local TAF concentration exceeds a predefined threshold and an adjacent lattice site contains an EC, a new vessel segment is created in the neighbouring empty site, mimicking sprout extension. When two sprouts meet, a loop is closed, and the interior is assumed to be perfused. The simulation visualises the progressive infiltration of vessels toward the tumour core, the branching of sprouts, and the eventual formation of a chaotic, poorly organised vascular network typical of aggressive tumours.
While the model captures the qualitative pattern of sprouting angiogenesis, it is heavily simplified. It neglects haemodynamic forces (pressure gradients, shear stress), the mechanical heterogeneity of the extracellular matrix, and the dynamic feedback between blood flow and endothelial cell survival. Parameter values (diffusion coefficients, decay rates, threshold concentrations) are chosen arbitrarily without reference to experimental measurements, limiting reproducibility and quantitative validation. Moreover, the authors provide only qualitative visual outputs; no quantitative metrics (e.g., vessel density, invasion depth, growth rate) are reported, nor is there any comparison with in‑vivo or in‑vitro data. Consequently, the model’s predictive power for therapeutic interventions or for understanding the kinetics of angiogenesis remains unclear.
In the discussion, the authors acknowledge these limitations and suggest future extensions: incorporation of hybrid continuous‑discrete frameworks to model fluid dynamics, sensitivity analysis of model parameters, and validation against histological images of tumour vasculature. They also propose that integrating anti‑angiogenic drug effects (e.g., VEGF inhibitors) could transform the CA into a tool for pre‑clinical testing of treatment strategies.
Overall, the paper succeeds in summarising the biological underpinnings of tumour angiogenesis and demonstrates that a minimalist CA can reproduce the hallmark features of sprouting vessels. However, to move beyond illustrative purposes, the model requires substantial refinement, rigorous parameter grounding, and systematic validation against experimental data.
Comments & Academic Discussion
Loading comments...
Leave a Comment