Detection of Metallo-b{eta}-Lactamases-Encoding Genes Among Clinical Isolates of Escherichia Coli in a Tertiary Care Hospital, Malaysia
The multidrug resistant Escherichia coli strains causes multiple clinical infections and has become a rising problem globally. The metallo-\b{eta}-lactamases encoding genes are very severe in gram-negative bacteria especially E. coli. This study was aimed to evaluate the prevalence of MBLs among the clinical isolates of E. coli. A total of 65 E. coli isolates were collected from various clinical samples of Malaysian patients with bacterial infections. The conventional microbiological test was performed for isolation and identification of E. coli producing MBLs strains in this vicinity. Multidrug Resistance (MDR) of E. coli isolates were assessed using disk diffusion test. Phenotypic methods, as well as genotypic- PCR methods, were performed to detect the presence of metallo-\b{eta}-lactamase resistance genes (blaIMP, blaVIM) in imipenem resistant strains. Out of 65 E. coli isolates, 42 isolates (57.3%) were MDR. The isolates from urine (19) produced significantly more MDR (10) isolates than other sources. Additionally, 19 (29.2%) imipenem resistant E. coli isolates contained 10 MBLs gene, 7(36.8%) isolates contained blaIMP and 3(15.7%) isolates contained blaVIM genes. This study revealed the significant occurrence of MBL producing E. coli isolates in clinical specimens and its association with health risk factors indicating an alarming situation in Malaysia. It demands an appropriate concern to avoid failure of treatments and infection control management.
💡 Research Summary
The study investigated the prevalence of metallo‑β‑lactamase (MBL)–encoding genes among clinical Escherichia coli isolates collected from a tertiary care hospital in Malaysia. A total of 65 non‑duplicate E. coli strains were obtained from a variety of clinical specimens (urine, wound, respiratory tract, stool, sputum, and blood) between November 2018 and February 2019. Species identification was confirmed by 16S rRNA PCR using universal primers. Antimicrobial susceptibility testing was performed by the Kirby‑Bauer disc diffusion method according to CLSI 2017 guidelines, employing twelve commonly used antibiotics, including β‑lactams, carbapenems, fluoroquinolones, and β‑lactam/β‑lactamase inhibitor combinations. Multidrug‑resistance (MDR) was defined as resistance to three or more antimicrobial classes. The results showed that 42 isolates (65 %) were MDR, with especially high resistance rates to cefalexin (89.2 %), cefepime (86.1 %), cefotaxime (83.6 %) and aztreonam (78.4 %). Nineteen isolates (29.2 %) were resistant to imipenem, a carbapenem of last resort.
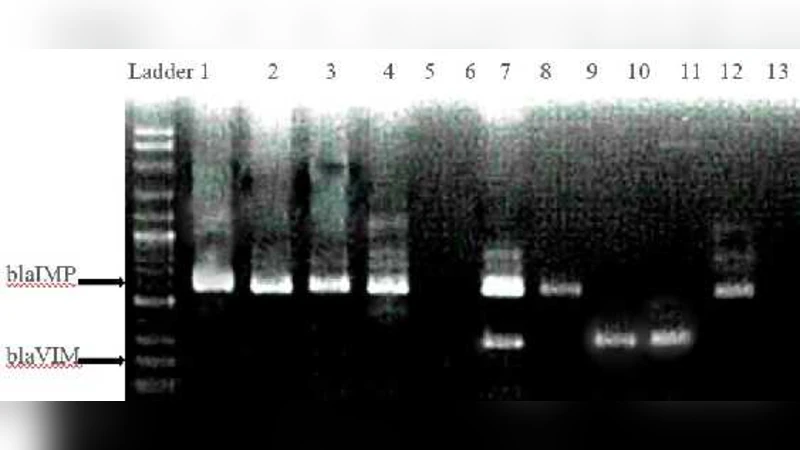
To detect MBL production, four phenotypic assays were employed: Modified Hodge Test (MHT), Double‑Disc Synergy Test (DDST), Combined Disc Test (CDT) with imipenem plus EDTA, and an E‑test strip containing imipenem and imipenem‑EDTA. Ten isolates (15.4 % of the total) yielded positive results in at least one phenotypic method. These ten isolates were subjected to PCR for the two most common MBL genes, blaIMP (587 bp) and blaVIM (261 bp). Seven isolates harbored blaIMP, three harbored blaVIM, and none carried both genes.
The distribution of MDR isolates by specimen type revealed that urine isolates contributed the highest proportion (30.9 % of MDR strains), followed by respiratory samples (21.4 %) and stool (4.7 %). The predominance of blaIMP over blaVIM aligns with reports from other Southeast Asian countries, where IMP‑type MBLs are more prevalent. Notably, only about half of the imipenem‑resistant isolates possessed an MBL gene, indicating that other carbapenem‑resistance mechanisms—such as KPC, NDM, ESBLs, or AmpC β‑lactamases—are likely present but were not investigated in this work.
The authors acknowledge several limitations: the modest sample size, the single‑center design, and the lack of detailed clinical data (e.g., prior antibiotic exposure, length of hospital stay, patient outcomes). Consequently, the findings cannot be generalized to the national level, and the statistical significance of observed differences was not rigorously tested.
In conclusion, the study provides evidence that MBL‑producing E. coli, particularly IMP‑type, are circulating in Malaysian clinical settings and contribute to carbapenem resistance. The detection of these genes underscores the need for enhanced antimicrobial stewardship, routine surveillance for carbapenemase producers, and infection‑control measures to curb the spread of multidrug‑resistant organisms. Future research should involve multicenter surveillance, whole‑genome sequencing to elucidate clonal relationships and mobile genetic elements, and comprehensive phenotypic and genotypic profiling of all carbapenem‑resistance mechanisms.
Comments & Academic Discussion
Loading comments...
Leave a Comment