Using mobile phone sensor technology for mental health research: Integrated analysis to identify hidden challenges and potential solutions
Background: Mobile phone sensor technology has great potential in providing behavioral markers of mental health. However, this promise has not yet been brought to fruition. Objective: The objective of our study was to examine challenges involved in developing an app to extract behavioral markers of mental health from passive sensor data. Methods: Both technical challenges and acceptability of passive data collection for mental health research were assessed based on literature review and results obtained from a feasibility study. Socialise, a mobile phone app developed at the Black Dog Institute, was used to collect sensor data (Bluetooth, global positioning system, and battery status) and investigate views and experiences of a group of people with lived experience of mental health challenges (N=32). Results: On average, sensor data were obtained for 55% (Android) and 45% (iPhone OS) of scheduled scans. Battery life was reduced from 21.3 hours to 18.8 hours when scanning every 5 minutes with a reduction of 2.5 hours or 12%. Despite this relatively small reduction, most participants reported that the app had a noticeable effect on their battery life. In addition to battery life, the purpose of data collection, trust in the organization that collects data, and perceived impact on privacy were identified as main factors for acceptability. Conclusions: Based on the findings of the feasibility study and literature review, we recommend a commitment to open science and transparent reporting and stronger partnerships and communication with users. Sensing technology has the potential to greatly enhance the delivery and impact of mental health care. Realizing this requires all aspects of mobile phone sensor technology to be rigorously assessed.
💡 Research Summary
**
The paper investigates the promise and the current shortcomings of using mobile phone sensor technology for mental health research, focusing on both technical and acceptability challenges. The authors developed and deployed “Socialise,” a native Android and iOS application created by the Black Dog Institute, to collect passive sensor data—Bluetooth, GPS, and battery status—from a sample of 32 participants who have lived experience of mental health difficulties. Over a four‑week period, the app performed scans at intervals of 3, 4, 5, or 8 minutes, uploading encrypted and hashed data to a secure server.
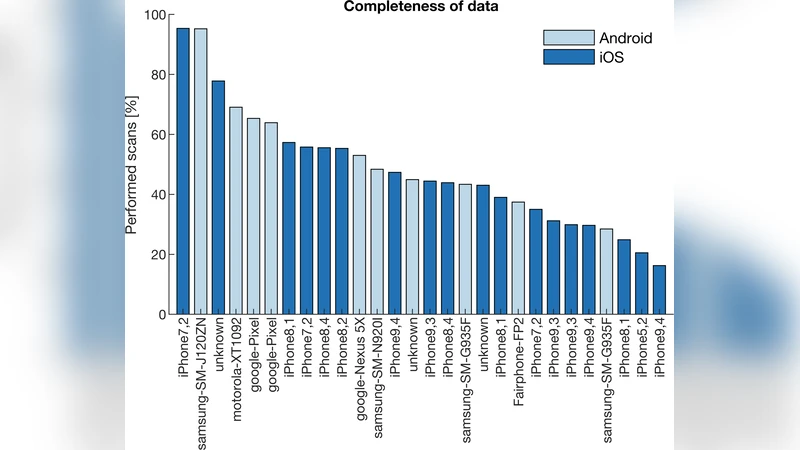
Key quantitative findings show that the Android version achieved an average data capture rate of 55 % of scheduled scans, whereas the iOS version captured only 45 %. This discrepancy is attributed to iOS’s stricter background execution policies and the lack of a low‑energy Bluetooth API, which limited continuous passive data collection. Battery consumption was also a notable issue: scanning every five minutes reduced average device uptime from 21.3 hours to 18.8 hours—a 2.5‑hour (≈12 %) decrease. Although the absolute reduction appears modest, the majority of participants reported a perceptible impact on battery life, indicating that even small energy costs can affect user willingness to continue participation.
Beyond raw technical metrics, the study explored participants’ attitudes toward data collection. Three factors emerged as primary determinants of acceptability: (1) clarity of the research purpose, (2) trust in the institution conducting the study, and (3) perceived privacy impact. Participants felt more comfortable when they were informed that data would be anonymized through hashing, that the research organization was reputable, and that the data would be used solely for scientific purposes. Conversely, any ambiguity about data handling or potential misuse heightened privacy concerns and reduced willingness to keep the app active.
The authors discuss several interrelated challenges. First, cross‑platform sensor access differences demand platform‑specific engineering solutions; for iOS, leveraging the Significant‑Change Location Service mitigated some data loss, but Bluetooth data remained sporadic. Second, battery life constraints necessitate a balance between sampling frequency and energy efficiency, suggesting the need for adaptive scanning schedules, on‑device preprocessing, and compressed transmission. Third, ethical transparency is essential: the authors advocate for open‑science practices, including public repositories of de‑identified data, detailed consent forms, and ongoing communication with participants about data use.
In the discussion, the paper emphasizes that successful deployment of passive sensor technologies in mental health hinges on a user‑centered design approach. Even though the app required minimal active input, participants still valued clear onboarding, real‑time feedback on battery consumption, and reassurance that the app operated unobtrusively in the background. The authors recommend establishing stronger partnerships with end‑users, clinicians, and ethicists to co‑design future iterations, thereby improving both data quality and participant retention.
Overall, the study validates that mobile phone sensors can capture behavioral markers relevant to mental health (e.g., social connectivity via Bluetooth proximity, mobility patterns via GPS), but practical implementation is limited by platform restrictions, energy demands, and privacy perceptions. The authors conclude that realizing the full potential of mobile sensing for mental health will require rigorous technical assessment, transparent reporting, and sustained engagement with the communities whose data are being collected. Future work should explore multimodal sensor fusion, machine‑learning‑driven marker extraction, and longer‑term longitudinal studies to strengthen the evidence base for clinical translation.
Comments & Academic Discussion
Loading comments...
Leave a Comment