Feasibility of sensor-based technology for monitoring health in developing countries - cost analysis and user perception aspects
Understanding the financial burden of chronic diseases in developing regions still remains an important economical factor which influences the successful implementation of sensor based applications for continuous monitoring of chronic conditions. Our research focused on a comparison of literature-based data with real costs of the management and treatment of chronic diseases in a developing country, and we are using Kosovo as an example here. The results reveal that the actual living costs exceed the minimum expenses that chronic diseases impose. Following the potential of a positive economic impact of sensor based platforms for monitoring chronic conditions, we further examined the users perception of digital technology. The purpose of this paper is to present the varying cost levels of treating chronic diseases, identify the users concerns and requirements towards digital technology and discuss issues and challenges that the application of sensor based platforms imply in low and middle income countries.
💡 Research Summary
**
The paper investigates the feasibility of deploying sensor‑based health‑monitoring technologies in low‑ and middle‑income countries, using Kosovo as a case study. It combines a quantitative cost analysis of chronic disease management with a qualitative assessment of user perceptions among patients and health‑care professionals.
First, the authors outline the burden of chronic diseases worldwide, noting that they account for roughly 80 % of deaths in developing regions and are projected to affect up to 65 % of the population by 2030. In Kosovo, the public health budget is limited: 51 % of the Ministry of Health’s funds go to hospitals, 26 % to municipalities, and the remaining 22 % to other expenses. Only half of the total health‑care costs are covered by the government; the other half is paid out‑of‑pocket by patients. A single rural visit for chronic‑disease care costs between €50 and €200 (including travel), while the average monthly wage is about €300. Basic living expenses (utilities, food, transport) total roughly €300 as well, meaning that health expenditures can exceed a household’s disposable income, especially given Kosovo’s high unemployment rate.
Second, the paper evaluates two commercially available sensor solutions: the Zephyr wireless heart‑rate monitor (€65) and the ZIO cardiac patch (€440). Although the upfront price of these devices is higher than a single clinic visit, the authors argue that the devices are a one‑time investment that can reduce the frequency of in‑person appointments, enable continuous home monitoring, and allow clinicians to intervene early when physiological parameters deviate from normal ranges. Citing studies from the United States and other settings, they show that hospitals employing advanced health‑information technologies experience fewer complications, shorter lengths of stay, and lower overall costs. The authors therefore posit that, over time, sensor‑based platforms could offset their initial cost through reduced travel, fewer hospital admissions, and improved disease management.
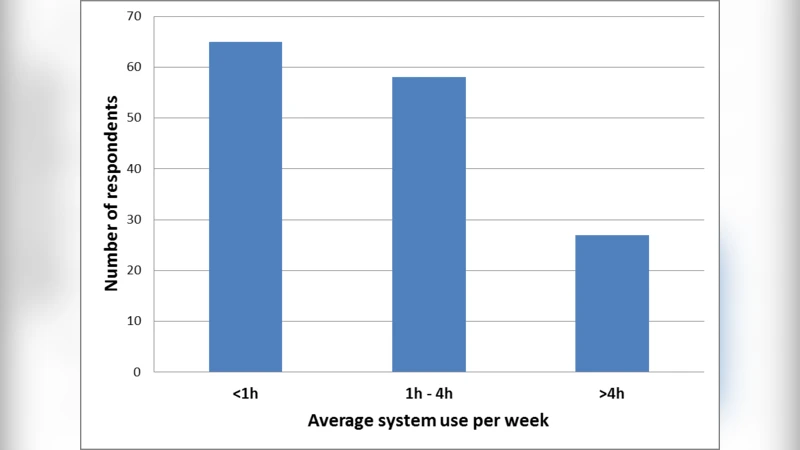
Third, the study surveys user acceptance. Both patients and health‑care staff express concerns about data privacy, the complexity of operating devices, lack of technical support, and the financial burden of purchasing sensors. Older adults and low‑income individuals are particularly hesitant due to limited digital literacy and smartphone ownership. Nonetheless, Kosovo’s internet penetration is relatively high (76.6 %), suggesting that the necessary connectivity infrastructure exists. Positive attitudes are linked to the promise of reduced travel, faster feedback, and greater autonomy in managing health.
The discussion highlights several implementation challenges: (1) the need for policy measures such as subsidies or leasing schemes to lower the initial cost barrier; (2) establishment of robust data‑security standards and reliable mobile/network infrastructure; (3) development of training programs for patients and clinicians to build digital competence; and (4) culturally sensitive design of user interfaces and communication strategies to build trust.
In conclusion, the authors demonstrate that chronic‑disease treatment costs in Kosovo exceed ordinary living expenses, creating a substantial economic strain on households. Sensor‑based remote monitoring offers a promising avenue to alleviate this burden by decreasing the number of costly clinic visits and enabling early clinical intervention. However, successful deployment hinges on addressing financial, technical, and socio‑cultural barriers. The insights derived from Kosovo are presented as a transferable framework for other low‑ and middle‑income nations seeking to integrate digital health solutions into their chronic‑care strategies.
Comments & Academic Discussion
Loading comments...
Leave a Comment