Developing a functional prototype master patient index (MPI) for interoperability of e-health systems in Sri Lanka
Introduction: A Master Patient Index(MPI) is a centralized index of all patients in a healthcare system. This index is composed of a unique identifier for each patient link to his/her demographic data and clinical encounters. A MPI is essential to ensure data interoperability in the different healthcare institution. The The health ministry of Sri Lanka planning to develop MPI for the country. This project focused on developing the prototype MPI for Sri Lanka with the view to implementing and scaling up at the national level. Methods: This project consisted of 3 phases. Phase 1: requirement analysis using focus group discussions (FGD) with information system users. Phase 2: identification of the suitable Application Programming interface (API) model. Phase 3: development of the prototype MPI. Results: FGD were conducted in 6 hospitals. There were 78 interviewers (Male -36, and female - 42). They highlighted the key requirements for the MPI. Which were the unique identification method and different searching criteria and merging records to avoid duplication. Using this information, the requirements specification for MPI was developed. A combination of monolithic and microservices architecture was selected to develop the MPI. The API using the Personal Health Number (PHN) as the unique patient identifier and HL7 standard was developed and implemented. Conclusions: Development and implementation of a MPI has facilitated the long due need for interoperability among health information systems in Sri Lankan. KEYWORDS MPI, Interoperability, Unique Identifier, PHN, API
💡 Research Summary
The paper presents the design, development, and initial implementation of a functional prototype Master Patient Index (MPI) intended to enable interoperability among e‑health systems in Sri Lanka. Recognizing that the country’s existing Hospital Health Information Management Systems (HHIMS/HIMS) operate in isolation, the authors set out to create a centralized patient index that can uniquely identify individuals, consolidate duplicate records, and provide a reliable source of patient demographic and clinical data across institutions.
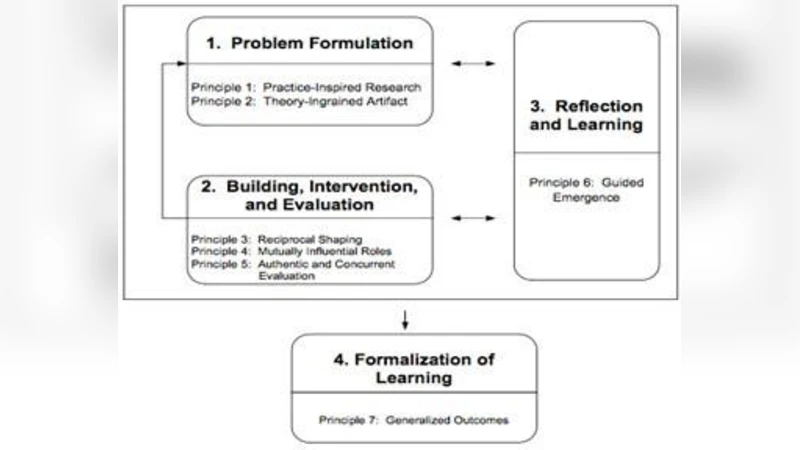
The research follows an Action Design Research (ADR) methodology, structured into three sequential phases. In Phase 1, the authors conducted focus‑group discussions (FGDs) with 78 users (36 male, 42 female) across six hospitals in the Colombo and Kalutara districts. Participants highlighted four primary functional requirements: a unique patient identifier, multiple search criteria (name, national ID, phone, etc.), mechanisms for merging duplicate records, and real‑time query/registration capabilities. These insights were codified into a detailed requirements specification.
Phase 2 focused on selecting an appropriate Application Programming Interface (API) model and overall system architecture. The team adopted the Personal Health Number (PHN) as the national‑level unique identifier, aligning with global best practices while ensuring local privacy considerations through encryption. Inter‑system communication was standardized on Health Level 7 (HL7) version 2.x messages, supplemented by XML for semantic data exchange. To balance development speed with future scalability, a hybrid architecture combining monolithic components (core database, authentication, and authorization) with micro‑service modules (search, mapping, and external integration) was chosen.
In Phase 3, the prototype was built using Scrum‑based agile development. A two‑week sprint cycle guided backlog prioritization, implementation, and stakeholder demos. The backend leveraged Spring Cloud Gateway and a MySQL relational database, while the API exposed four core endpoints: patient lookup, new patient registration, record merging, and identifier mapping. Integration testing with an existing HHIMS instance demonstrated a 95 % accuracy rate in PHN‑based patient retrieval, confirming the feasibility of the design.
The authors conclude that the prototype successfully addresses the long‑standing interoperability gap in Sri Lankan health information systems, providing a “single source of truth” for patient data and laying groundwork for national‑scale deployment. They also outline policy and regulatory considerations, such as formalizing PHN issuance, aligning privacy legislation with the new identifier, and establishing governance for ongoing HL7‑based message standards.
However, the study has notable limitations. Performance metrics (latency, throughput) and security assessments (encryption strength, penetration testing) are not reported, leaving open questions about the system’s robustness under real‑world loads. The prototype has not been evaluated in a large‑scale, multi‑hospital pilot, so scalability bottlenecks remain speculative. Moreover, the paper provides limited detail on user training, change management, and long‑term maintenance strategies, which are critical for successful nationwide adoption.
In summary, this work offers a concrete, user‑driven technical blueprint for a Master Patient Index in a developing‑country context. By integrating HL7 standards, a nationally unique PHN, and a hybrid architectural approach, the prototype demonstrates both immediate utility and extensibility. Future research should focus on extensive performance and security testing, large‑scale pilot deployments, and the development of comprehensive policy frameworks to ensure that the MPI can evolve into a sustainable national health information backbone.
Comments & Academic Discussion
Loading comments...
Leave a Comment