Effect of Statistical Fluctuation in Monte Carlo Based Photon Beam Dose Calculation on Gamma Index Evaluation
The gamma-index test has been commonly adopted to quantify the degree of agreement between a reference dose distribution and an evaluation dose distribution. Monte Carlo (MC) simulation has been widely used for the radiotherapy dose calculation for both clinical and research purposes. The goal of this work is to investigate both theoretically and experimentally the impact of the MC statistical fluctuation on the gamma-index test when the fluctuation exists in the reference, the evaluation, or both dose distributions. To the first order approximation, we theoretically demonstrated in a simplified model that the statistical fluctuation tends to overestimate gamma-index values when existing in the reference dose distribution and underestimate gamma-index values when existing in the evaluation dose distribution given the original gamma-index is relatively large for the statistical fluctuation. Our numerical experiments using clinical photon radiation therapy cases have shown that 1) when performing a gamma-index test between an MC reference dose and a non-MC evaluation dose, the average gamma-index is overestimated and the passing rate decreases with the increase of the noise level in the reference dose; 2) when performing a gamma-index test between a non-MC reference dose and an MC evaluation dose, the average gamma-index is underestimated when they are within the clinically relevant range and the passing rate increases with the increase of the noise level in the evaluation dose; 3) when performing a gamma-index test between an MC reference dose and an MC evaluation dose, the passing rate is overestimated due to the noise in the evaluation dose and underestimated due to the noise in the reference dose. We conclude that the gamma-index test should be used with caution when comparing dose distributions computed with Monte Carlo simulation.
💡 Research Summary
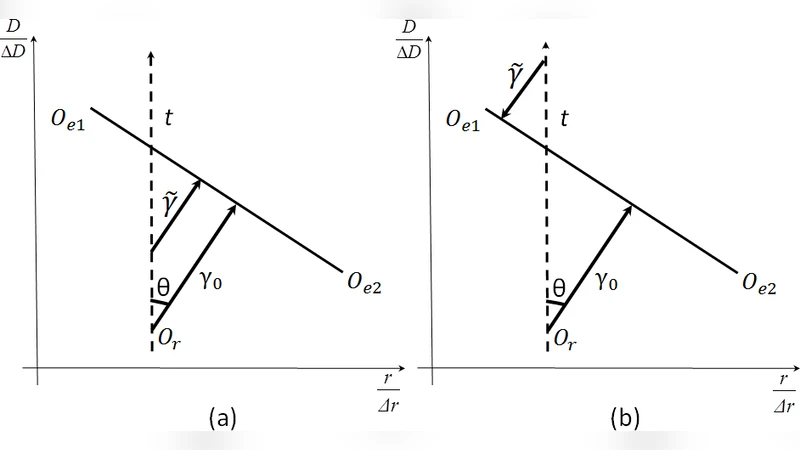
The paper investigates how statistical fluctuations inherent to Monte Carlo (MC) dose calculations affect the gamma‑index (γ‑index) test, a widely used metric for quantifying agreement between a reference dose distribution and an evaluation dose distribution in radiotherapy. The authors first develop a simplified analytical model in which Gaussian noise is added independently to the reference dose (D_ref) and the evaluation dose (D_eval). By expanding the γ‑index definition (γ = max{ΔD/ΔD_crit, r/r_crit}) to first order, they show that when the original γ value is relatively large (i.e., the two distributions differ appreciably), noise in the reference dose tends to increase γ, whereas noise in the evaluation dose tends to decrease γ. This theoretical result predicts opposite biases depending on which distribution carries the MC statistical uncertainty.
To validate the theory, the authors conduct numerical experiments using clinical photon therapy cases (lung, breast, and prostate). For each patient, they generate dose distributions with a conventional deterministic algorithm (e.g., AAA or Acuros) and with a high‑fidelity MC engine (egsnrc). The MC dose is deliberately degraded to three levels of relative standard deviation (0.5 %, 1 %, and 2 %) by reducing the number of simulated particles, thereby creating controlled amounts of statistical noise. Gamma‑index analyses are performed under two common criteria: 3 %/3 mm and 2 %/2 mm.
Three comparison scenarios are examined:
-
MC reference vs. non‑MC evaluation – As the noise level in the MC reference increases, the mean γ value rises and the passing rate (percentage of points with γ ≤ 1) declines. This indicates that MC‑derived reference doses appear more discrepant than they truly are, leading to a conservative (over‑stringent) quality‑assurance outcome.
-
Non‑MC reference vs. MC evaluation – In this configuration, the average γ value drops and the passing rate climbs as the MC evaluation noise grows, provided the γ values lie within the clinically relevant range. The MC noise effectively masks real differences, producing an overly optimistic assessment of agreement.
-
MC reference vs. MC evaluation – When both distributions contain noise, the two opposing effects partially cancel. However, if the reference noise exceeds the evaluation noise, the overall passing rate is reduced; the opposite bias occurs when the evaluation noise dominates.
These findings confirm the theoretical prediction and reveal a fundamental limitation of the γ‑index: it does not intrinsically account for the statistical uncertainty of the input dose maps. Consequently, the test can both over‑estimate and under‑estimate agreement depending on where the MC noise resides.
The authors discuss practical implications. When MC simulations are used as the gold‑standard reference, sufficient particle histories must be simulated to keep statistical uncertainty below about 0.5 % or a noise‑correction term should be incorporated into the γ‑calculation. When MC doses serve as the evaluation distribution, clinicians must recognize that the passing rate may be artificially inflated and consider either matching the noise level of the reference or reporting confidence intervals that reflect MC uncertainty. In the case of mutual MC comparison, a “noise‑matching” procedure—ensuring comparable statistical variance in both datasets—helps mitigate bias.
In conclusion, while MC dose calculation remains the most accurate physical model for photon beam therapy, its statistical fluctuations can significantly distort γ‑index outcomes. The paper urges caution in interpreting γ‑index results involving MC data and recommends systematic noise management or correction to preserve the reliability of treatment‑plan verification.