Sodium Magnetic Resonance Imaging: Biomedical Applications
In this article, we present an up-to-date overview of the potential biomedical applications of sodium MRI in vivo. Sodium MRI is a subject of increasing interest in translational research as it can give some direct and quantitative biochemical information on the tissue viability, cell integrity and function, and therefore not only help the diagnosis but also the prognosis of diseases and treatment outcomes. It has already been applied in vivo in most of human tissues, such as brain for stroke or tumor detection and therapeutic response, in breast cancer, in articular cartilage, in muscle and in kidney, and it was shown in some studies that it could provide very useful new information not available through standard proton MRI. However, this technique is still very challenging due to the low detectable sodium signal in biological tissue with MRI and hardware/software limitations of the clinical scanners. The article is divided in three parts: (1) the role of sodium in biological tissues, (2) a short review on sodium magnetic resonance, and (3) a review of some studies on sodium MRI on different organs/diseases to date.
💡 Research Summary
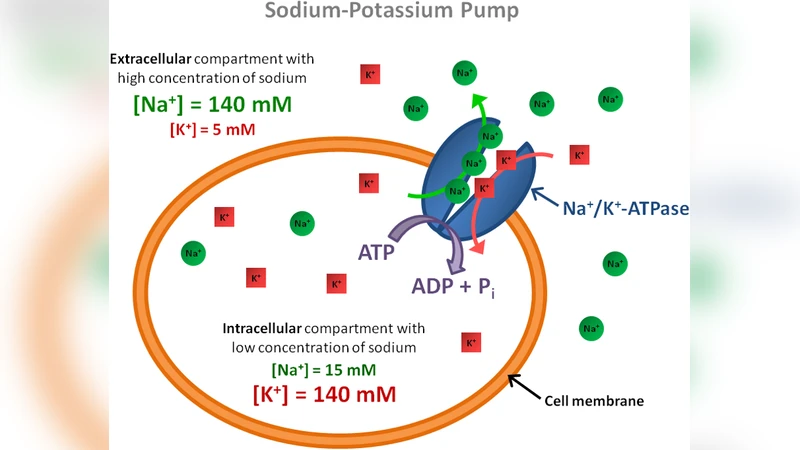
The reviewed article provides a comprehensive overview of sodium magnetic resonance imaging (23Na MRI) and its emerging biomedical applications. Sodium ions, present in both extracellular (~140 mM) and intracellular (~10 mM) compartments, serve as direct reporters of cell viability, membrane integrity, and metabolic activity because their concentration changes sensitively with alterations in cell volume, ion transport, and tissue perfusion. Unlike conventional proton (1H) MRI, sodium MRI can therefore deliver quantitative biochemical information that is otherwise inaccessible.
From a physics standpoint, 23Na possesses a spin‑3/2 nucleus, resulting in a relatively low gyromagnetic ratio (≈26 % of 1H) and a complex relaxation behavior characterized by a short T2 component (2–5 ms) and a longer component (15–30 ms). These properties demand high‑performance hardware: dedicated multi‑channel sodium coils, high‑power RF amplifiers, ultra‑short echo time (UTE) or 3‑D spiral‑in (SPI) sequences, and sophisticated B1‑field mapping for non‑uniformity correction. Quantitative imaging further requires external reference phantoms or internal calibration to convert signal intensity into absolute sodium concentration.
Clinically, the article surveys the most compelling in‑vivo studies across several organ systems. In acute cerebral ischemia, sodium accumulation precedes conventional diffusion changes, offering a potential early marker of cytotoxic edema and a tool for monitoring reperfusion therapies. Brain tumor investigations demonstrate that elevated sodium correlates with cellular density and proliferative activity, enabling assessment of treatment response. In breast cancer, high‑sodium regions improve lesion characterization when combined with standard 1H MRI. Articular cartilage studies exploit the linear relationship between sodium concentration and glycosaminoglycan (GAG) content, allowing non‑invasive detection of early osteoarthritic degeneration. Muscular applications include tracking sodium shifts after exercise or in neuromuscular disorders, reflecting intracellular‑extracellular ion redistribution. Renal imaging shows promise for evaluating sodium handling abnormalities in acute kidney injury and chronic disease. Across these examples, sodium MRI consistently provides “new information” that complements conventional imaging, enhancing diagnostic confidence and prognostic assessment.
Despite its promise, the technique remains technically demanding. The intrinsic low signal‑to‑noise ratio (SNR) forces long acquisition times (often 10–20 minutes for whole‑organ coverage) and limits spatial resolution. Standardization of acquisition protocols, post‑processing pipelines, and normative sodium concentration databases is still lacking, hindering multi‑center reproducibility. Moreover, the need for specialized coils and sequence packages adds cost and complexity to routine clinical workflows.
Future directions highlighted include the deployment of ultra‑high‑field scanners (≥7 T) to boost SNR, the development of multi‑band transmit/receive systems that can simultaneously acquire 1H and 23Na data, and the integration of compressed sensing and deep‑learning reconstruction algorithms to accelerate scans without sacrificing image quality. Such advances are expected to reduce scan times, improve resolution, and facilitate quantitative mapping, paving the way for sodium MRI to become a routine biomarker in precision medicine, drug development, and tissue‑engineering research.
In summary, sodium MRI offers a unique window into tissue biochemistry, with demonstrated utility in neuro‑, oncologic, musculoskeletal, and renal imaging. Overcoming current hardware and methodological barriers will be essential for its broader clinical adoption, but the potential to provide direct, quantitative insights into cellular health makes it a compelling frontier in modern medical imaging.
Comments & Academic Discussion
Loading comments...
Leave a Comment