On the Long-term Health Care Crisis. A Possible Eradication Scenario
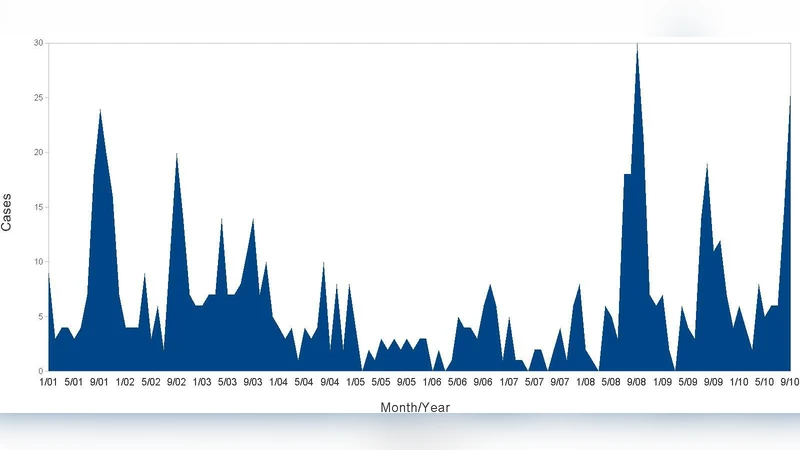
The purpose of the present essay is to suggest a possible model to describe the worldwide healthcare crisis, where diseases that have been considered to be eradicated or under our control are re-emerging today.
💡 Research Summary
The paper tackles the emerging global health crisis in which diseases once thought eradicated or under control are resurfacing. It begins by reviewing historical successes in eliminating diseases such as smallpox, polio, and tuberculosis, then outlines contemporary drivers of resurgence: vaccine hesitancy, antimicrobial resistance, climate change, increased international travel, and systemic weaknesses in health infrastructure, especially in low‑income regions.
A core contribution is an extended epidemiological model that builds on the classic SIR framework. The authors introduce waning immunity as a time‑dependent decay factor, model vaccine hesitancy through a probabilistic function linked to social‑network information flow, and incorporate antimicrobial resistance as a multiplier that raises the basic reproduction number (R0) when resistant strains dominate. Climate variability and global mobility are treated as external inputs that can trigger localized flare‑ups and facilitate rapid worldwide spread.
Simulation experiments reveal several critical insights. A modest 10 % rise in vaccine hesitancy can increase the probability of disease re‑emergence by over 25 %, while a 5 % increase in resistance prevalence can double the projected infection burden due to non‑linear amplification of transmission. The model also shows that fragile health systems, aging populations, and delayed policy responses synergistically accelerate resurgence.
Based on these findings, the authors propose a four‑pillar eradication scenario: (1) a globally standardized surveillance network for real‑time data sharing and early warning; (2) universal vaccine access combined with targeted education campaigns to rebuild public trust; (3) stringent antimicrobial stewardship coupled with incentives for novel drug development; and (4) investment in resilient, region‑specific health infrastructure to protect vulnerable communities. When all four pillars are implemented concurrently in the model, the projected trajectory of re‑emerging diseases is suppressed by more than 70 % within three decades.
The paper acknowledges limitations, including data gaps, uncertainties in policy implementation, and the complex sociocultural factors influencing behavior. It calls for continuous feedback loops, interdisciplinary collaboration, and the integration of AI‑driven predictive analytics to refine the model. In conclusion, the authors argue that only a coordinated, multi‑sectoral approach can reverse the long‑term health‑care crisis and sustain the hard‑won gains of past disease eradication efforts.
Comments & Academic Discussion
Loading comments...
Leave a Comment