Intercellular spiral waves of calcium in a two dimensional network of cells
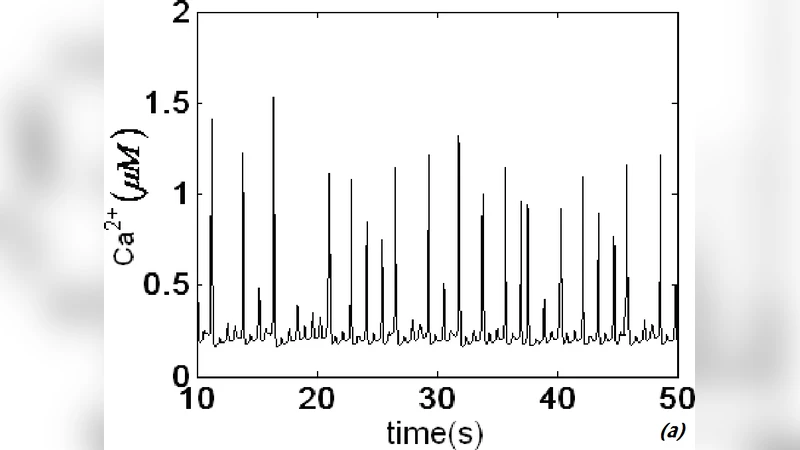
It is shown, by means of numerical simulations, that intercellular spiral waves of calcium can be initiated in a network of coupled cells as a result of a de-synchronization between Ca2+ oscillations in two domains. No artificial heterogeneities need to be imposed to the system for spontaneous formation of spiral waves. The de-synchronization occurs near the interface of the stimulated region (which acts as a pacemaker) and propagates over the entire network. We also find the outcome of the collision of two spiral waves.
💡 Research Summary
The paper presents a computational study of intercellular calcium (Ca²⁺) dynamics in a two‑dimensional lattice of coupled cells, demonstrating that spiral‑shaped calcium waves can arise spontaneously without imposing any artificial heterogeneity. Each cell is modeled as a minimal Ca²⁺ oscillator that includes IP₃‑dependent release from the endoplasmic reticulum, SERCA‑mediated reuptake, and exchange with the extracellular space. Cells are linked to their nearest neighbors through diffusive coupling, which represents gap‑junctional calcium fluxes.
A localized region of the lattice is continuously stimulated by fixing a high intracellular IP₃ concentration, thereby turning that region into a persistent pacemaker. The pacemaker oscillates with a fixed period and drives the surrounding non‑stimulated cells. At the interface between the stimulated and non‑stimulated domains a phase mismatch develops: the pacemaker cells fire earlier, while the adjacent cells lag behind. This mismatch produces a local desynchronization that propagates outward and gives rise to a rotating wave front.
Systematic parameter sweeps reveal that the strength of diffusive coupling (denoted D) is critical. For very low D the wave cannot leave the stimulated zone; for very high D the entire lattice becomes synchronized and the spiral pattern disappears. In an intermediate window (approximately D ≈ 0.1–0.2 in nondimensional units) a stable spiral wave forms, with its core located near the pacemaker boundary. The core drifts only slowly, while the rotation period and wavelength remain essentially constant.
The authors also explore the interaction of two spirals that are generated either simultaneously or sequentially. When the wave fronts collide, several outcomes are observed: (i) mutual annihilation of the colliding arms, (ii) survival of one spiral with the other extinguished, and (iii) formation of a new spiral with a shifted core. The post‑collision dynamics are quantified by measuring calcium concentration fields and phase maps before and after impact. These behaviors mirror experimental observations of colliding calcium waves in cultured epithelial sheets and cardiac tissue.
Boundary conditions play a decisive role. With periodic boundaries the spirals can circulate indefinitely, producing a lattice‑wide rotating pattern. Fixed (no‑flux) boundaries cause wave fronts to reflect, generating complex interference patterns and sometimes leading to secondary spiral nucleation near the edges. This sensitivity to geometry underscores the relevance of the model to real tissues, where physical constraints such as tissue edges or extracellular matrix anchoring affect wave propagation.
In summary, the study establishes three key points: (1) A homogeneous network of calcium‑oscillating cells can self‑organize into spiral waves solely through the combination of a localized pacemaker and diffusive coupling; (2) Desynchronization at the pacemaker‑non‑pacemaker interface is the mechanistic seed for spiral core formation; (3) Spiral‑spiral collisions produce a rich repertoire of outcomes that can be predicted by the same set of equations.
These findings have broad implications for understanding wave‑based pathologies such as ventricular tachycardia, cortical spreading depression, and coordinated epithelial contractions. By identifying the minimal conditions required for spiral wave emergence, the work provides a theoretical foundation for strategies aimed at controlling or eliminating pathological calcium waves, for example through targeted modulation of gap‑junction conductance or localized pharmacological alteration of IP₃ signaling.
Comments & Academic Discussion
Loading comments...
Leave a Comment