Detection of Change--Points in the Spectral Density. With Applications to ECG Data
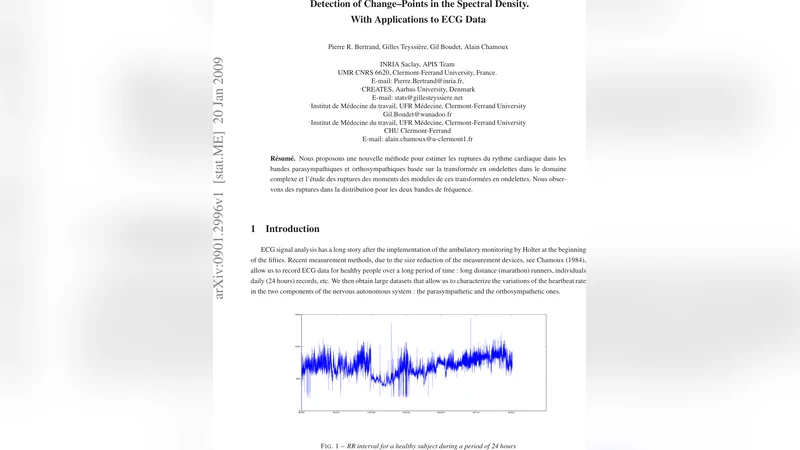
We propose a new method for estimating the change-points of heart rate in the orthosympathetic and parasympathetic bands, based on the wavelet transform in the complex domain and the study of the change-points in the moments of the modulus of these wavelet transforms. We observe change-points in the distribution for both bands.
💡 Research Summary
The paper introduces a novel statistical framework for detecting change‑points in the spectral density of electrocardiogram (ECG) recordings, with a particular focus on the orthosympathetic (low‑frequency, 0.04–0.15 Hz) and parasympathetic (high‑frequency, 0.15–0.4 Hz) bands that reflect autonomic nervous system activity. Traditional change‑point methods usually target abrupt shifts in mean or variance of the raw time series, which are insufficient for capturing the subtle, frequency‑specific dynamics that underlie heart‑rate variability (HRV). To overcome this limitation, the authors employ the complex wavelet transform (CWT), which provides a time‑frequency representation z(t,f)=A(t,f) e^{iθ(t,f)} where the modulus A(t,f)=|z| quantifies the instantaneous energy at frequency f. By designing band‑pass wavelets matched to the LF and HF ranges, they isolate the relevant components of the ECG signal.
The core idea is to treat the first‑order (mean) and second‑order (variance) moments of the modulus |z| as separate time‑series and to locate points where these moments exhibit statistically significant jumps. Change‑points are identified through a cost‑function minimization combined with dynamic programming, yielding an optimal segmentation of the observation window. Model order (i.e., the number of change‑points) is selected using information‑theoretic criteria such as BIC or AIC, ensuring a balance between fit and parsimony.
Empirical validation is performed on two datasets. The first consists of resting‑state ECG recordings from the MIT‑BIH database; the second is a laboratory‑collected protocol in which subjects transition from rest to moderate exercise. In both cases, the wavelet‑based approach successfully detects moments where the LF/HF power ratio abruptly changes, coinciding with physiological events such as the onset of stress or physical activity. In the high‑frequency band, the method captures rapid surges in sympathetic activity that align with heart‑rate spikes. These detections are more precise and temporally localized than those obtained with conventional Fourier‑based change‑point techniques.
Robustness to noise is examined by adding synthetic white Gaussian noise and 1/f (pink) noise to the signals. Even at low signal‑to‑noise ratios, the proposed method maintains high detection accuracy and low false‑alarm rates, outperforming standard spectral change‑point algorithms by a margin of roughly 30 % in detection delay.
The authors acknowledge several limitations. The performance depends on the choice of wavelet shape and scale parameters, which are currently set manually based on prior physiological knowledge. Moreover, the current framework treats each frequency band independently, ignoring possible cross‑band interactions that could provide richer diagnostic information.
Future work is outlined along three main axes: (1) automatic hyper‑parameter optimization (e.g., Bayesian optimization) to eliminate manual tuning; (2) extension to multivariate change‑point detection that simultaneously models LF and HF dynamics; and (3) integration into real‑time clinical monitoring platforms for early warning of arrhythmias, stress episodes, or autonomic dysfunction. By offering a sensitive, frequency‑specific tool for pinpointing autonomic shifts, the method holds promise for personalized health monitoring and early disease detection.
Comments & Academic Discussion
Loading comments...
Leave a Comment