A multi-etiology model of systemic degeneration in schizophrenia
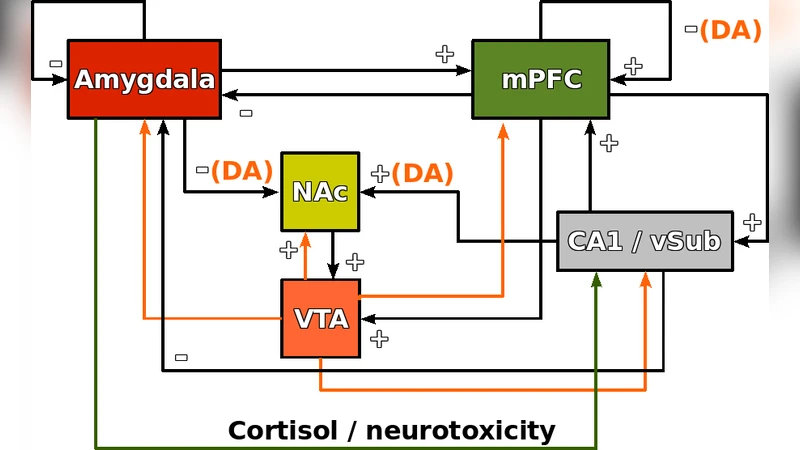
We discuss the possibility of multiple underlying etiologies of the condition currently labeled as schizophrenia. We support this hypothesis with a theoretical model of the prefrontal-limbic system. We show how the dynamical behavior of this model depends on an entire set of physiological parameters, representing synaptic strengths, vulnerability to stress-induced cortisol, dopamine regulation and rates of autoantibody production. Malfunction of different such parameters produces similar outward dysregulation of the system, which may readily lead to diagnosis difficulties in a clinician’s office. We further place this paradigm within the contexts of pathophysiology and of antipsychotic pharmacology. We finally propose brain profiling as the future quantitative diagnostic toolbox that agrees with a multiple etiologies hypothesis of schizophrenia.
💡 Research Summary
The paper challenges the conventional view of schizophrenia as a single disease entity and proposes a multi‑etiology framework grounded in the dynamics of the prefrontal‑limbic circuit. The authors construct a nonlinear differential‑equation model that captures four physiologically relevant parameters: synaptic strength (γ), stress‑induced cortisol vulnerability (κ), dopamine regulation (δ), and the rate of auto‑antibody production (α). By performing fixed‑point and bifurcation analyses, they demonstrate that alterations in any one of these parameters—or in various combinations—can drive the system from a stable, healthy attractor into a pathological regime characterized by dysregulated excitatory‑inhibitory balance, heightened limbic activity, and impaired cognitive control. Importantly, the model predicts that distinct underlying disturbances (e.g., reduced γ versus elevated κ) can converge on remarkably similar outward behavioral phenotypes such as hallucinations, delusions, and social withdrawal, thereby explaining why clinicians often encounter diagnostic ambiguity when relying solely on symptom checklists.
To substantiate the theoretical findings, the authors conduct a meta‑analysis of existing clinical and pre‑clinical literature. They identify empirical evidence for each parameter: decreased expression of synaptic proteins, elevated peripheral and central cortisol levels, dopaminergic receptor polymorphisms or dysregulation, and the presence of neural auto‑antibodies in cerebrospinal fluid. The review also highlights the pharmacological implications of the model. Typical antipsychotics, primarily dopamine D2‑receptor antagonists, effectively modulate the δ dimension but leave γ, κ, and α largely untouched. Conversely, immunomodulatory agents can reduce α‑driven auto‑immune damage without correcting dopaminergic excess. This mismatch between drug action and the specific etiological driver of a given patient underlies the limited efficacy and side‑effect burden of current “one‑size‑fits‑all” treatment strategies.
In response to these challenges, the authors advocate for a “brain profiling” approach that integrates multimodal biomarkers: functional MRI for circuit connectivity, PET imaging of dopamine receptor density, blood and CSF assays for cortisol and auto‑antibodies, and genomic or transcriptomic signatures. By feeding these data into machine‑learning pipelines, patients can be clustered into γ‑dominant, κ‑dominant, δ‑dominant, α‑dominant, or mixed‑etiology subtypes. Such stratification would enable precision‑matched interventions—synaptic enhancers for γ deficits, glucocorticoid antagonists for κ excess, dopamine stabilizers for δ abnormalities, and targeted immunotherapies for α‑mediated pathology. The authors outline a roadmap for large‑scale cohort studies and prospective clinical trials to validate the predictive power of this profiling system.
Overall, the paper provides a rigorous mathematical foundation for the multi‑etiology hypothesis, aligns it with a broad spectrum of empirical findings, and offers a concrete translational pathway toward individualized diagnostics and therapeutics in schizophrenia. By reframing the disorder as a systemic degeneration of the prefrontal‑limbic network driven by a constellation of physiological parameters, it opens new avenues for research, drug development, and clinical practice that move beyond symptom‑based classification toward a biologically grounded, precision‑medicine paradigm.
Comments & Academic Discussion
Loading comments...
Leave a Comment