Pressure sensor-based tongue-placed electrotactile biofeedback for balance improvement - Biomedical application to prevent pressure sores formation and falls
We introduce the innovative technologies, based on the concept of “sensory substitution”, we are developing in the fields of biomedical engineering and human disability. Precisely, our goal is to design, develop and validate practical assistive biomedical and/or technical devices and/or rehabilitating procedures for persons with disabilities, using artificial tongue-placed tactile biofeedback systems. Proposed applications are dealing with: (1) pressure sores prevention in case of spinal cord injuries (persons with paraplegia, or tetraplegia); and (2) balance control improvement to prevent fall in older and/or disabled adults. This paper describes the architecture and the functioning principle of these biofeedback systems and presents preliminary results of two feasibility studies performed on young healthy adults.
💡 Research Summary
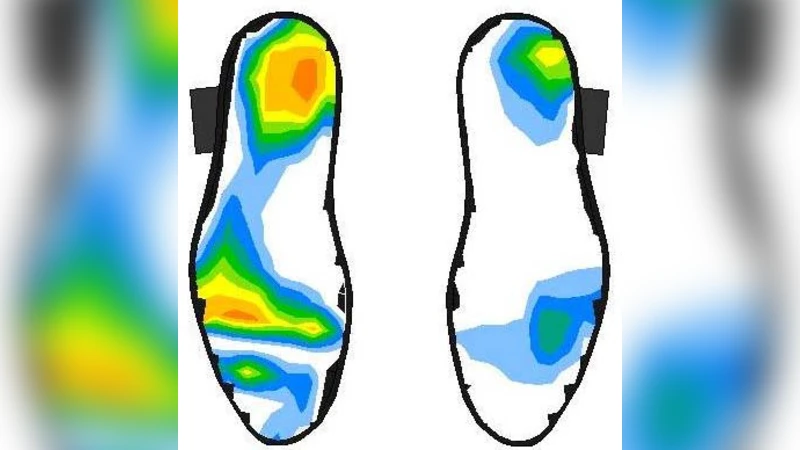
The paper presents a novel bio‑feedback platform that exploits the concept of sensory substitution by delivering electrotactile cues to the tongue. The system consists of a matrix of 36 surface electrodes (6 × 6) mounted on a thin, biocompatible oral insert, a wireless communication module, a rechargeable battery, and one or more sensor units that capture either pressure distribution (for pressure‑sore prevention) or body sway (for balance enhancement). In the pressure‑sore application, pressure sensors embedded in a seat or mattress continuously monitor the user’s load pattern. When a region exceeds a predefined safety threshold, an algorithm translates the location and magnitude of the overload into a specific activation pattern on the tongue‑electrode array. The user perceives a localized tingling sensation that intuitively signals the direction of excessive pressure, prompting a weight shift or postural adjustment before tissue damage can develop.
For balance control, foot‑pressure sensors combined with an inertial measurement unit (IMU) estimate the user’s anterior‑posterior and medial‑lateral tilt angles. These tilt estimates are mapped onto the electrode matrix so that a tilt to the right, for example, produces a left‑side tongue stimulus. The user can therefore correct the sway without relying on visual or auditory cues, which is especially valuable for older adults or individuals with visual impairments.
The hardware architecture is deliberately compact: the sensor module transmits data via low‑latency Bluetooth Low Energy, the processing unit runs a lightweight risk‑detection algorithm, and the electrotactile driver delivers low‑amplitude (≤5 V) pulses that are safe for oral tissue. The battery provides roughly eight hours of continuous operation, and the whole system can be donned and removed in under a minute.
Preliminary feasibility was assessed with ten healthy young adults. In the pressure‑feedback trial, participants correctly identified overload zones 85 % of the time, with an average reaction time of 1.2 seconds after stimulus onset. In the balance‑feedback trial, subjects performed a blind‑folded stance on a sway‑platform; the presence of tongue feedback reduced the standard deviation of trunk sway by about 30 % compared with the no‑feedback condition (p < 0.01). These results demonstrate that the tongue can serve as an effective conduit for rapid, intuitive tactile information.
The authors acknowledge several limitations. The spatial resolution of the 6 × 6 electrode grid constrains the granularity of conveyed information, and individual differences in lingual sensitivity require adaptive calibration. Prolonged use may cause mucosal fatigue or dryness, and the current wireless latency (up to 200 ms) plus battery endurance may restrict long‑term daily use. Future work will explore higher‑density electrode arrays, machine‑learning‑based personalization of stimulus patterns, and more ergonomic oral substrates. Crucially, the next phase will involve clinical trials with spinal‑cord‑injured patients and elderly participants to validate efficacy in real‑world settings.
In summary, the tongue‑placed electrotactile biofeedback system offers a non‑invasive, real‑time method for delivering critical somatosensory information, with promising applications in pressure‑sore prevention for individuals with paraplegia or tetraplegia and in fall‑prevention for older adults. By converting otherwise inaccessible pressure or balance data into a perceptible lingual cue, the technology bridges a sensory gap and opens new avenues for assistive rehabilitation devices.
Comments & Academic Discussion
Loading comments...
Leave a Comment